
The rapid ascent of glucagon-like peptide-1 (GLP-1) receptor agonists has fundamentally altered the landscape of metabolic medicine, sparking a global conversation about the necessity of traditional lifestyle interventions in an era of pharmaceutical weight loss. While the initial cultural narrative suggested that medications like Ozempic and Wegovy might render the gym obsolete, a landmark study published in the journal Sports Medicine provides a definitive rebuttal. The research, a secondary analysis of data from the University of Copenhagen, underscores a critical clinical reality: while GLP-1 drugs are peerless at reducing body mass, they cannot replicate the multifaceted physiological benefits of physical exercise. Without a concurrent fitness regimen, patients risk losing significant muscle mass and failing to improve their functional health, potentially trading one set of health risks for another.
The Evolution of Weight Management Pharmacology
To understand the significance of the latest findings, one must look at the trajectory of GLP-1 agonists. Originally developed to treat type 2 diabetes, these medications mimic a hormone naturally produced in the intestines that signals satiety to the brain and slows gastric emptying. The massive success of semaglutide (marketed as Ozempic for diabetes and Wegovy for obesity) led to a surge in prescriptions and a shift in public perception regarding weight loss.
However, as the "honeymoon phase" of these drugs transitions into long-term clinical observation, medical professionals have raised alarms regarding "sarcopenic obesity"—a condition where individuals lose weight but also lose a disproportionate amount of lean muscle tissue. This loss of muscle can lead to a lower metabolic rate, decreased bone density, and diminished physical strength. The University of Copenhagen study, funded in part by the Novo Nordisk Foundation, sought to address whether these negative outcomes could be mitigated through a structured exercise program.
Study Methodology and Chronology
The research team, led by scientists at the University of Copenhagen in Denmark, utilized a rigorous four-arm randomized controlled trial design. The study followed 193 adults, aged 18 to 65, all of whom were classified as having obesity (a body mass index between 32 and 43).
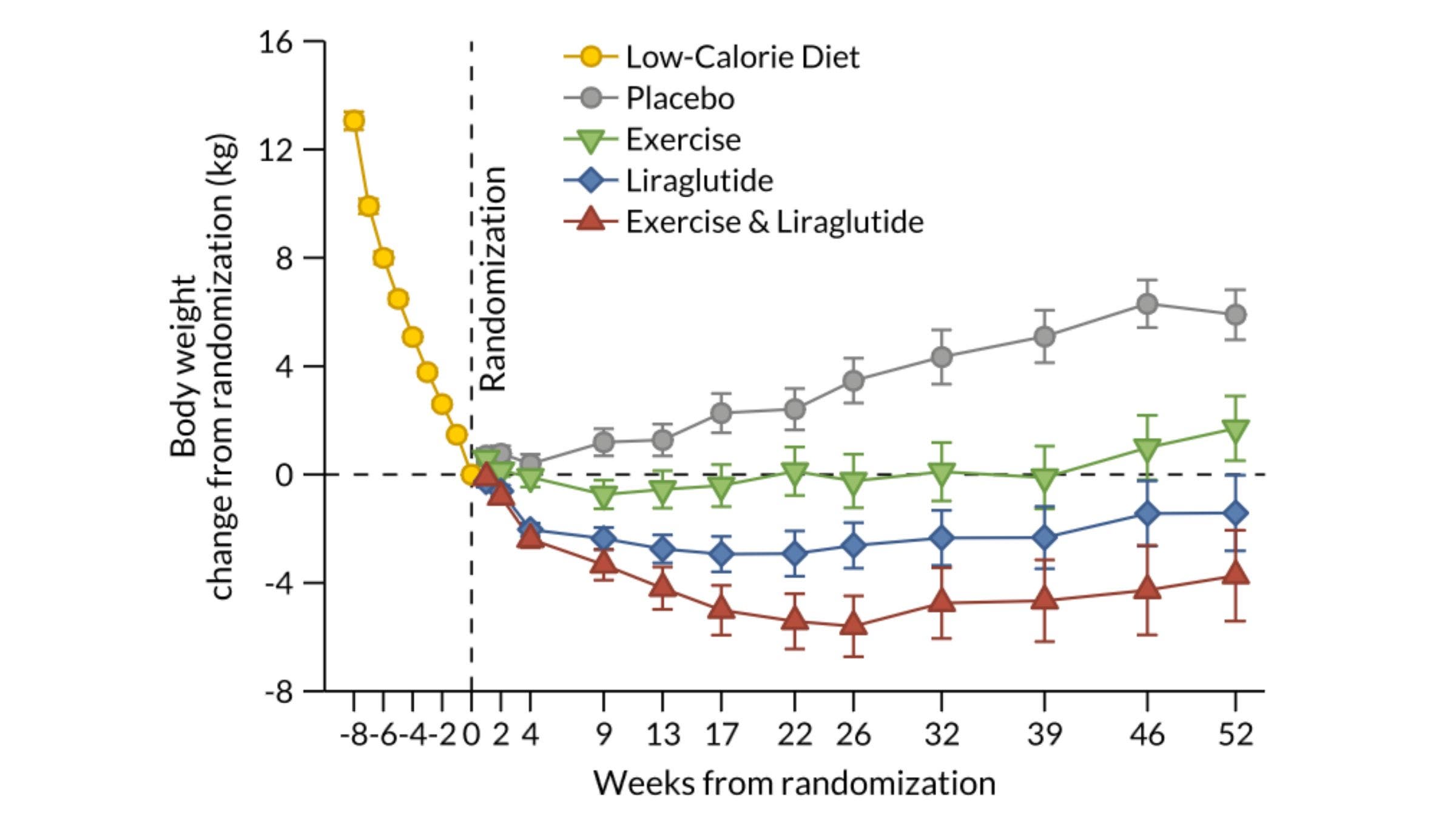
The experiment began with an intensive eight-week lead-in phase. During this period, all participants followed a very-low-calorie diet (approximately 800 calories per day), resulting in an average weight loss of 13.1 kilograms (roughly 29 pounds), or about 12 percent of their initial body weight. This phase was designed to ensure that the subsequent year-long study focused on the maintenance of weight loss rather than the initial drop.
Following the initial weight loss, participants were divided into four distinct groups for a 52-week maintenance period:
- The Placebo Group: Received a placebo injection and maintained their usual activity levels.
- The Exercise-Only Group: Followed a supervised exercise program without GLP-1 medication.
- The Medication-Only Group: Received daily injections of liraglutide (a GLP-1 agonist sold as Saxenda or Victoza) but did not follow a structured exercise plan.
- The Combination Group: Received both the GLP-1 medication and followed the structured exercise program.
The exercise protocol was robust, designed to meet and exceed standard public health guidelines. It consisted of two supervised group sessions per week, featuring 30 minutes of high-intensity interval training (HIIT) on indoor cycles followed by 15 minutes of circuit training involving step-ups, squats, and kettlebell exercises. Participants were also encouraged to complete two additional individual sessions per week, such as running or brisk walking.

Comparative Data: Weight Maintenance and Body Composition
The results of the year-long maintenance phase revealed a clear hierarchy of effectiveness. The placebo group, as expected, regained a significant portion of the weight lost during the initial eight-week diet. In contrast, both the exercise-only and medication-only groups were successful in maintaining their weight loss, though the medication-only group showed a slight statistical edge in total poundage kept off.
However, the "Combination Group" (medication plus exercise) emerged as the clear winner. These participants not only maintained their initial weight loss but continued to lose additional weight throughout the year. More importantly, the quality of their weight loss was superior. By combining the appetite-suppressing effects of the GLP-1 drug with the metabolic demands of exercise, these individuals were able to maximize fat loss while preserving—and in some cases increasing—their lean muscle mass.
The study highlighted a concerning trend in the medication-only group. While they remained "thin," their body composition metrics suggested a decline in relative muscle quality. This finding corroborates growing clinical concerns that GLP-1 drugs, when used in a vacuum, may result in "skinny fat" phenotypes where the individual has a healthy BMI but lacks the muscular strength necessary for long-term metabolic health.
Functional Fitness and the Stair-Climb Metric
Beyond simple weight measurements, the Danish researchers focused on functional fitness—the ability to perform everyday physical tasks. One of the primary tools used was the stair-climb test, which required participants to ascend and descend an 11-step stairway twice as quickly as possible.
The data from this test provided a stark contrast between the groups. Participants in the exercise and combination groups showed significant improvements in their stair-climb times, indicating better cardiovascular health and lower-body power. Conversely, those in the medication-only group showed virtually no improvement in functional speed, despite being significantly lighter than they were at the start of the study.
This disparity underscores the "Fit vs. Fat" paradox. Historically, epidemiological data has suggested that an individual who is overweight but aerobically fit often has a lower risk of cardiovascular death than an individual who is of normal weight but sedentary. The Copenhagen study suggests that GLP-1 drugs can solve the "fatness" half of the equation, but only exercise can solve the "fitness" half.
Comprehensive Physiological Outcomes
The secondary analysis published in Sports Medicine delved deeper into aerobic capacity, measured via VO2 max (the maximum amount of oxygen the body can utilize during intense exercise). VO2 max is widely considered the gold standard for cardiorespiratory fitness and is a powerful predictor of longevity.
The findings were consistent across multiple metrics:
- Aerobic Power: The exercise and combination groups saw marked increases in VO2 max. The medication-only group saw their absolute VO2 max remain stagnant or decline, though their relative VO2 max (adjusted for body weight) improved slightly because they were carrying less mass.
- Skeletal Muscle Mass: Dual-energy X-ray absorptiometry (DXA) scans revealed that the combination group preserved twice as much muscle mass as the medication-only group.
- Metabolic Markers: While all groups taking the GLP-1 drug saw improvements in blood glucose and insulin sensitivity, the combination group showed the most significant reductions in systemic inflammation markers and improved lipid profiles.
Expert Reactions and Clinical Implications
The medical community has reacted to these findings with a call for a "lifestyle-first" or "lifestyle-integrated" approach to GLP-1 prescriptions. Dr. Signe Torekov, a lead author of the study and professor at the University of Copenhagen, emphasized that the goal of weight loss should be "healthy weight loss," which necessitates the maintenance of physical function.
"It is a common misconception that these drugs are a ‘get out of jail free’ card for exercise," noted one independent metabolic specialist not involved in the study. "This data proves that if you use the drug to lose weight but remain sedentary, you are essentially a smaller, weaker version of your previous self. You haven’t necessarily improved your underlying vitality."
The pharmaceutical industry has also taken note. There is an increasing focus on developing "next-generation" GLP-1s or adjunct therapies that specifically target muscle preservation. However, as the Danish study suggests, the most effective "adjunct therapy" is already available in the form of resistance and aerobic training.
Broader Impact and the Future of Obesity Treatment
The implications of this research extend to public health policy and insurance coverage. As healthcare systems grapple with the high cost of GLP-1 medications, there is a growing argument that these drugs should be prescribed alongside supervised exercise programs to ensure the best long-term outcomes for patients.
Furthermore, the study challenges the "diet culture" obsession with the scale. By shifting the focus to functional tests like the stair-climb and VO2 max, the researchers are advocating for a more holistic definition of health. For the millions of people currently taking GLP-1 agonists, the message is clear: the medication is a powerful tool for weight management, but it is not a replacement for the biological necessity of movement.
As we move deeper into the 2020s, the "Ozempic era" is likely to be defined not just by the drugs themselves, but by how we integrate them into traditional health practices. The Copenhagen study serves as a vital reminder that while science can manufacture a hormone that makes us less hungry, it cannot manufacture the strength, stamina, and resilience that come from physical exertion. For those seeking the maximum benefit from modern medicine, the treadmill and the weight rack remain as essential as the needle.






